Key Takeaways
- The ACCESS Model offers significantly lower reimbursement rates ($180–$420/year) compared to traditional RPM and CCM programs ($1,500–$2,400/year).
- Enrollment in ACCESS creates “billing exclusivity,” preventing practices from billing traditional FFS codes for the same chronic conditions.
- New Outcome-Aligned Payments (OAPs) include a 50% upfront withhold, which is only paid back if specific clinical outcomes are demonstrated after 12 months.
- Practices face financial penalties through “substitute spend adjustments” if patients receive fragmented care from outside providers for the same condition.
- The most viable strategy for most PCPs is to maintain FFS billing while capturing incremental revenue through the $30 ACCESS co-management payment.
Last week, we published an overview of the CMS ACCESS Model and why primary care physicians should understand it. Today, we want to give you the other side of that story — the one the CMS press release doesn’t lead with. Because if you’re a primary care doctor already running a solid RPM or CCM program, the honest answer to “should I join ACCESS?” is probably no. And understanding why will help you make a smarter decision about where your practice stands as Medicare continues shifting toward outcome-based reimbursement.
The Payment Rates Are Lower Than Anyone Expected
When CMS published the actual ACCESS payment figures in February 2026, the reaction across the digital health and primary care world was swift and largely critical. Here is what the numbers actually look like:
| Clinical Track | Annual OAP (Initial Period, per patient) |
|---|---|
| eCKM (hypertension, prediabetes, dyslipidemia, obesity) | $360/year |
| CKM (diabetes, ASCVD, chronic kidney disease) | $420/year |
| MSK (chronic musculoskeletal pain) | $180/year |
| Behavioral Health (depression, anxiety) | $180/year |
These are total allowed amounts — meaning they include both the 80% Medicare share and the 20% patient coinsurance. If you choose to waive coinsurance (which CMS encourages to improve patient access), you only collect 80% of those figures. And 50% of whatever you’d earn is withheld upfront, paid back only after you demonstrate outcomes at the end of the 12-month care period.
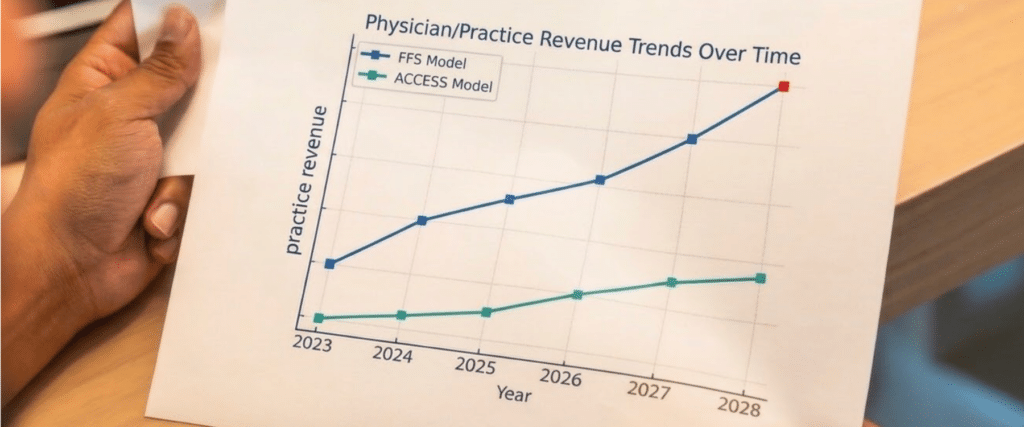
By comparison, a primary care practice running a properly structured RPM and CCM program for the same patients can generate — under current FFS billing — between $1,500 and $2,400 per active patient per year. That’s three to six times the ACCESS rate, with no outcome risk, no infrastructure mandate, and no billing exclusivity problem.
The Billing Exclusivity Problem Is a Real Risk
This is the piece that gets the least attention but matters most for practices already doing RPM or CCM. Under ACCESS, once a patient is enrolled in the program for a specific condition, the ACCESS participant — and any affiliated providers — cannot bill traditional Medicare fee-for-service codes for managing that same condition during the care period.
That means if you enroll your hypertensive patient in ACCESS, you lose the ability to bill 99454, 99457, 99458, or CCM codes for that patient’s hypertension for up to 14 months. You are trading a $1,800–$2,400 annual revenue stream for $288–$360 (after the coinsurance waiver and 50% holdback).
If one of your ACCESS-enrolled patients separately receives RPM services or care
management from another Medicare provider for the same condition, CMS reduces your
ACCESS payment. You are financially penalized for care fragmentation — even care you
didn’t order. Tracking this across a patient panel adds compliance burden with no additional
upside.
What the Industry Is Actually Saying
This is not a contrarian take. The industry reaction to the ACCESS payment rates has been unusually candid. Manatt health-tech legal expert Randi Seigel stated publicly that “the rates are quite low to motivate new entrants to the Medicare program given the infrastructure they need to compliantly operate the program and achieve the desired outcomes” — and that many initially interested companies would need to “take a hard look at the numbers to understand viability.”
The American Academy of Family Physicians has been equally measured, stating it is advocating to “make sure this model does not disrupt the physician-patient relationship.” That is a careful way of saying: primary care doctors are concerned that ACCESS pulls their chronic patients toward tech companies and away from the practice that actually knows them.
The model was designed primarily with digital health startups in mind — companies that are not currently Medicare-enrolled, have direct-to-consumer patient acquisition strategies, and can scale technology-enabled care across large populations at low marginal cost. That is a very different operating model than a primary care practice in New Jersey or Pennsylvania managing 1,500 Medicare patients.
So Who Should Actually Consider Joining ACCESS?
In fairness to the model, there are specific scenarios where ACCESS participation could make sense. They are narrow, but real.
1. Practices with no current chronic care management program
If a primary care practice is doing nothing structured for their chronic disease population today — no RPM, no CCM, no care coordination — ACCESS provides an incremental revenue stream from a population that is currently generating nothing beyond office visit billing. For those practices, $360 per hypertensive patient per year beats zero. But that is also exactly the population that should be talking to RPM Logix first, because the FFS model will generate significantly more revenue with less compliance risk. Click HERE to schedule a strategy call with RPM Logix.
2. Large health systems playing a positioning game
A major health system might absorb below-market ACCESS rates in exchange for visibility in CMS’s public participant directory, data infrastructure investment, and positioning if the model expands or rates increase. For an independent primary care practice, that calculus does not apply.
3. Practices interested in the co-management path
This is actually the most interesting option for most primary care doctors. Rather than becoming an ACCESS participant, a PCP can refer chronic patients to an ACCESS-enrolled organization, receive structured monthly clinical updates, and bill a new co-management payment of approximately $30 per review — up to roughly $100 per patient per year — without taking on any ACCESS compliance burden or losing FFS billing rights.
The Smart Play: Stay in FFS, Use the Co-Management Path
For the vast majority of primary care physicians currently running or considering an RPM or CCM program, the optimal strategy right now is straightforward:
- Keep your FFS RPM and CCM billing.
- Refer appropriate chronic patients to an ACCESS-enrolled organization to capture the co-management payment.
- Maintain full control of the physician-patient relationship and your practice’s revenue structure.
- Monitor ACCESS rate adjustments. CMS has committed to reviewing model performance annually. If rates increase meaningfully or the model goes permanent, the calculus changes.
RPM Logix provides clinical staff, monitoring infrastructure, and population health reporting that powers your RPM and CCM program under general supervision. Your practice bills Medicare directly and keeps the margin. Our Population Health Reporting and Analytics platform also generates the structured monthly clinical data that satisfies the ACCESS co-management payment documentation requirement — so your practice can capture that incremental revenue without adding workflow.
Whether ACCESS rates improve and make direct participation worthwhile in 2027 or 2028 is a question we’ll answer together as the data comes in. For now, the better-paying, lower-risk path runs through your current FFS program — supported by the right infrastructure.
The direction CMS is moving is clear and it is not reversing. Outcome-based reimbursement will eventually become the dominant framework for chronic care in Medicare. The practices that are building population health infrastructure today — real data, real monitoring, real care coordination — will be positioned to participate on their own terms when that transition arrives. ACCESS in its current form is not the hill to plant your flag on. But the preparation it demands is exactly what a well-run RPM program already delivers.
This article is part two of our series on the CMS ACCESS Model. Read HERE for part one: “The CMS ACCESS Model Explained: How Physicians Can Prepare for Medicare’s Shift to Outcome-Based Chronic Care.“
To learn how RPM Logix Population Health Reporting & Analytics helps physician practices maximize Medicare reimbursement under FFS while preparing for the future of outcome-based care, contact us at mario@rpmlogix.com.